I woke up with a spiking fever, and 38.0 C came quickly. Burning eyeballs again….I was uncomfortable. Any time that a patient goes above 38, the Team follows a protocol. I was examined, labs upon labs were drawn, given Tylenol and started on an IV dose of antibiotics. (For the record, I’m already taking a prophylactic anti-viral). The part that I cared the most about? Yes, IV meds rock, but with feeling uncomfortable and achy, Tylenol won out.
I texted Andy and the text chain that involves my folks and aunt Lucy, and promptly fell back asleep.
By 9 am, I was awake and getting my pre-chemo IV meds. This round of chemotherapy, the medication Cytoxan, only lasts two days (Day 3+ and 4+. By the way, I like the + signs, for the record, and most transplant patients use it as a reference). That being said, in order to prevent potential side effects, I need to be hooked up to IV fluids 24/7 and receive MENSA, a bladder protective medication. I also need to pee every two hours.
To remember, I set an alarm. And because I’m in the hospital, I came up with creative labels for said alarms:
And because it’s never just one or two things to manage, always four or nine, I was placed on Respiratory Isolation because of my slightly filling maxillary sinus for part of the day – basically the Penalty Box in hockey (I’m from MN, this is how we speak) – and my team also decided that I needed a blood transfusion in the form of Red Blood Cells only.


The blood cells were interesting. For my Stem Cell Transplant, I’m a perfect 8/8 match to my donor, but an overall 9/10, otherwise known as a “minor mismatch”, where his blood type O+ differs from my type A+. In transplants such as mine, a rare complication between days 4+ – 14+ can occur when the Patient’s body (that’s me!) attacks the donor stem cells. That’s bad bad bad. My Team will be able to tell that has occurred if my hemoglobin suddenly drops 3-ish points; this morning’s number of 8.8 was low enough to make a drop such as that life-threatening. So to be extra safe, something that I have zero problem with, the Team opted for a transfusion.
I’m lucky that I tolerated it well. I’m also on 2 or 3 different nausea meds because of the MENSA, but let’s not exclude. I am still nauseated, but have kept everything down. I just don’t really want to eat. The other good news, is that I’m no longer constipated. And I’ll leave it at that.
You’re welcome.
In other news along the lines of dropping blood counts, my platelets, those things in the blood that help us clot, have dropped below 100. (Again – totally planned with pre transplant chemo). My Lupron shot, which stops my period for a month, continued to bleed 5 minutes after the needle was pulled from the belly of my deltoid.

Another interesting thing is how my team is handling my history of blood clots. Before entering in-patient, I took Xarelto to prevent blood clots. Upon entering the NIH, I was place on a shot of Lovonox (liquid blood thinner). Now that my platelets are below 100, the Lovonox dose has decreased by 20 mg; when they drop below 50, I’ll be on heparin, another type of blood clot prevention.
And now, it’s late. I’ve been peeing all day. And I’ve had a witness.

Goodnight!


Your sense of humor uplifts and shines a steady beacon of hope and inspiration. I loved your alarm reminders – it’s the little things that give the pause for gratitude. Continued blessings and prayers surround you my friend. Your team is a group of Superheroes! Forget Marvel and DC. Team Marit ROCKS!
LikeLike
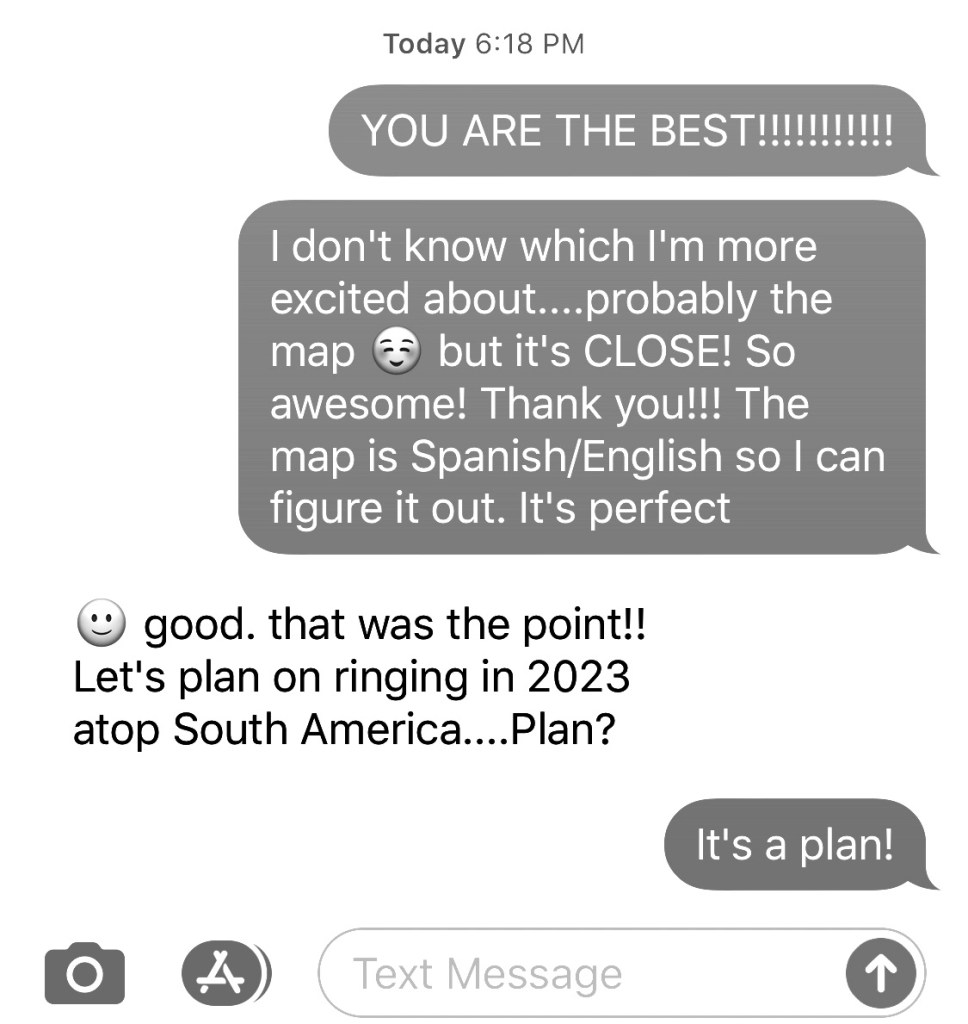
Oh – the ups and downs of a bone marrow transplant. Wonderful getting surprise from Christine – getting map of Aconcagua 🧗. I see you ringing in 2023 ✅✅ Getting pb & chocolate wasn’t bad either😊!! But the fever 🥵 wasn’t good – discomfort and all. Sorry. Thankful for Tylenol and transfusion. I marvel at your spirit and your strength. Oh, by the way, I’m baking this weekend.
LikeLike
Hi Marit,
You keep surprising me with your ability to complete these posts at the end of a long and trying day. And to do so in a witty manner. I’ve heard about your strength and courage and humor in the past, but you are providing plenty of evidence here. Happy Halloween! I hope there are some treats coming your way!
LikeLike
Great writing It’s amazing that you are so coherent and humorous In spite of all that is happening to you. The qualities you are showing will contribute to healthy life over the next 50+ years
Love Dad
LikeLike